 Physiotherapists are key healthcare professionals involved in the care of myeloma patients. They may be able to show patients different ways of sitting, sleeping, or moving to help them manage pain. They can also advise on safe ways to increase their activity or mobility.
Physiotherapists are key healthcare professionals involved in the care of myeloma patients. They may be able to show patients different ways of sitting, sleeping, or moving to help them manage pain. They can also advise on safe ways to increase their activity or mobility.
Here, Emily Mean, Clinical Specialist Myeloma Physiotherapist from Hampshire Hospitals NHS Foundation Trust, takes us through how the role of a myeloma physiotherapist has become embedded in clinical practice.
Funding of the role
Initial funding for the post was secured in 2015 from Hampshire Hospitals NHS Foundation Trust charitable funds, with the successful recruitment of a Band 7 physiotherapist in post in January 2019 for 17.5 hours per week. The post was made substantive in January 2021 following the restructuring of the inpatient haematology ward budget. Hours were increased to 21 hours per week, with additional ward management responsibilities added to the role to justify using the ward budget.
Day-to-day responsibilities
The myeloma physiotherapist provides a therapy service to the haematology ward at Basingstoke and North Hampshire Hospital.
The service focuses on maintaining and increasing physical function and conditioning during inpatient stays. It also provides rehabilitation following spinal cord compression or other complications secondary to malignant disease, comprehensive discharge planning and palliative care support.
A dedicated haematology/myeloma physiotherapy outpatient service provides face-to-face consultations, joint clinic visits with consultants and an outpatient rehabilitation service for patients with ongoing functional needs. Prehabilitation and rehabilitation pre- and post-transplant are also offered in inpatient and outpatient settings.
Strong links and working relationships with the Spinal Myeloma Clinic at Royal National Orthopaedic Hospital, Stanmore, and with local orthotic service at Hampshire Hospitals NHS Foundation Trust have ensured patients with spinal involvement are referred for specialist review and management.
The physiotherapist provides ongoing support, advice and liaison during the period of spinal management, including post-bracing exercise, support with returning to work, normal function and activity levels.
The post ensures all patients receive specialist therapy input into their care planning and overall management. It also allows onward referral to our Wellbeing and Supportive Care Service and includes psycho-oncology and complementary therapy.
Impact of the role
We have seen an uptake in the number of physiotherapy sessions delivered over the years.
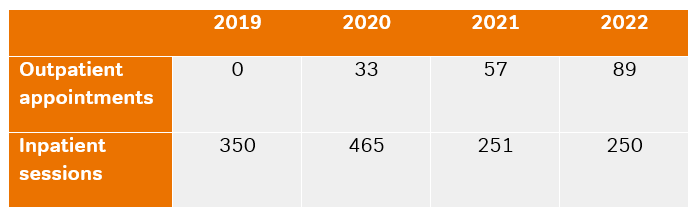
When Basingstoke and North Hampshire Hospital was accredited by the Myeloma UK Clinical Services Excellence Programme in 2022, the role of the Myeloma Physiotherapist was specifically mentioned in the final report.
Patient and carer feedback also demonstrates the impact of the role on individuals:
“Learning to walk again was the hardest thing I’ve done. We had weekly sessions to work on balance and build muscle strength back up, at the beginning I struggled to cycle for a minute and was so tired, but by the time I was discharged I was cycling 60 minutes!”
“The support we have both received from the physio has been amazing, we’re incredibly lucky to have a dedicated myeloma physiotherapist within our team and I truly believe my partner would not have made the progress he did without her. In the back of my mind I wasn’t 100% sure he’d be able to return to work as his role does involve a lot of walking, he now does anything between 14,000-18,000 steps a shift!”
“The physio was hugely supportive during my husband’s bracing treatment at Stanmore, during his rehab after a stem cell transplant and worked hard to build his confidence so he could return to work. The biggest impact she had was when he was nearing the end of his life. She went above and beyond anything we could have expected to buy coordinating equipment and liaising with his doctors to ensure everything was in place for his safe transfer back home.”
Next steps
Before the pandemic, a pilot ‘Myeloma Walk and Talk’ session was planned. The pilot will be a weekly walk around a short set circuit suitable for all abilities and with ample rest places along the way. The pilot will hopefully provide a springboard for developing a myeloma support group in Basingstoke (there is already one in Winchester for patients at the Royal Hampshire County Hospital) and for other cancer groups to be able to use the resources to start their own ‘Walk and Talk’.
Developing the Wellbeing and Supportive Care Service involves a Band 4 Rehabilitation Assistant Practitioner role. There is scope to further develop this role in supporting our myeloma and haematology patients, with advice on remaining physically active before, during and after treatment.
Written by Emily Mean
Clinical Specialist Myeloma Physiotherapist
Hampshire Hospitals NHS Foundation Trust






